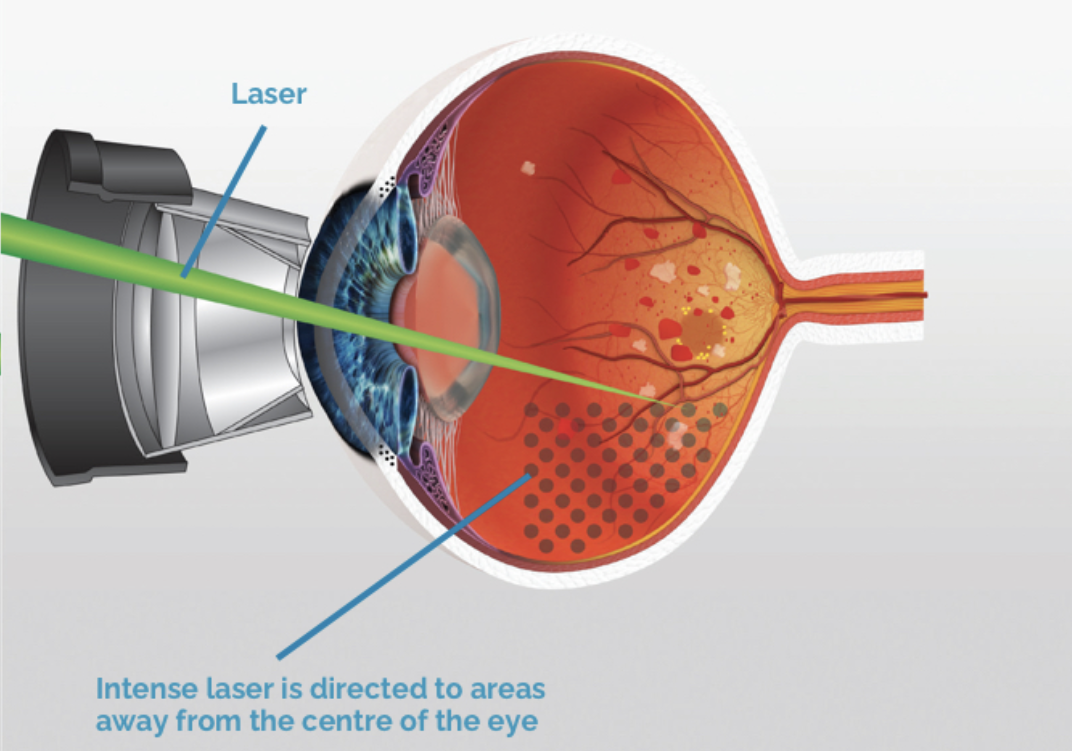 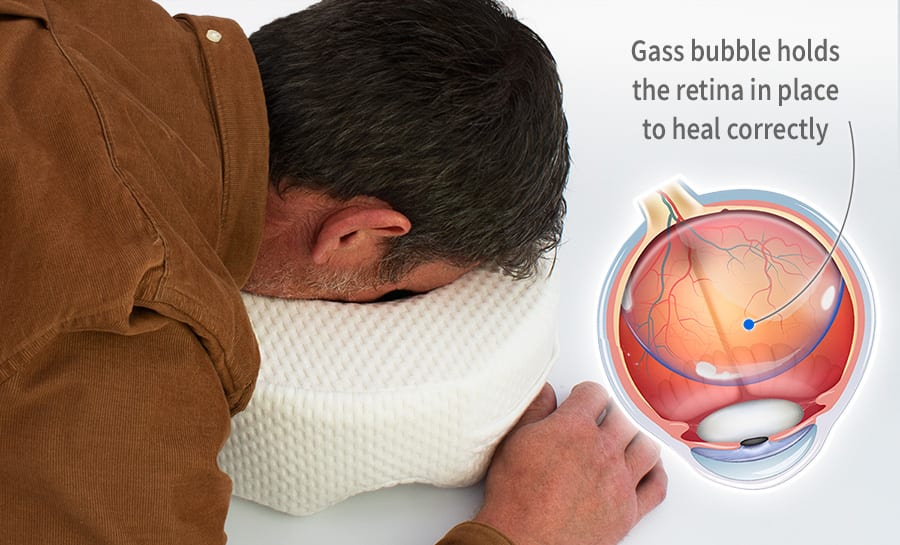
The premise was that tumors required a prominent blood supply to continue growing, and it was determined that this angiogenesis was a VEGF-mediated process. The idea of anti-VEGF medications comes from the oncology world. (I won’t discuss intravitreal or periocular steroid injections, because those are well known to cause an increase in IOP, and they’ve been extensively documented and discussed elsewhere.) In particular, I’ll discuss anti-VEGF injections, vitrectomy surgery with or without tamponade, the use of a scleral buckle and the use of panretinal photocoagulation laser. 
Here, I’d like to share some of what we know about this concern, the patients who may be at risk, and what we can do to prevent negative consequences from arising-and treat them if they do. For that reason, spreading awareness of this issue can be helpful. However, sometimes a patient is sent to a glaucoma specialist only after the pressure has been elevated for a while. Thus, to avoid glaucoma-related complications, it behooves us to identify patients who may be more susceptible to damage in this situation.Īs a retina specialist, I know that my glaucoma colleagues are aware of this issue, and there’s usually good communication between the retina and glaucoma teams. However, susceptibility to damage in some patients can cause even a brief rise in pressure to be consequential and in other patients, the brief pressure spike can be followed by a long-term IOP increase. In most cases, the increase is temporary, so although the pressure can become quite high, consequences are usually minimal or nonexistent. Unfortunately, many retina-related procedures, including anti-VEGF injections and some surgical interventions, can cause an increase in IOP. A s every ophthalmologist knows, elevated intraocular pressure is a risk factor for glaucoma progression.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
